TL;DR
Diabetes increases the risk of foot complications through nerve damage (neuropathy) and reduced circulation (ischaemia). Because these conditions can mask injuries and slow healing, consistent daily inspections are vital. Up to 80% of diabetes-related amputations are preventable with early intervention, such as professional callus removal and proper moisture management. If you notice non-healing wounds, spreading redness, or changes in skin colour, seek urgent medical attention from a podiatrist or your GP.
Living with diabetes requires a proactive approach to health, particularly when it comes to your feet. In the UK, diabetes is one of the leading causes of avoidable foot complications.
Managing diabetes means foot health is a critical priority. According to recent data from Diabetes UK, there are now more than 190 diabetes-related amputations every week in England, yet research suggests that up to 80% of these complications are preventable with early intervention and consistent care.
Important Note: This article is for informational purposes and is not a substitute for professional medical advice.
Why Diabetes Affects Your Feet
The NHS and Diabetes UK categorize the feet as a high-priority area because diabetes impacts the body in two specific ways that converge at the extremities:
1. Nerve Damage (Neuropathy)
Over time, high blood glucose levels can damage the small nerves in your feet. This often results in a loss of sensation. You may not feel a blister caused by a tight shoe, a small stone in your sock, or even a cut. Because the “pain signal” is missing, these minor injuries can go untreated and develop into ulcers.
2. Reduced Circulation (Ischaemia)
Diabetes can also affect blood flow. If your circulation is poor, your body struggles to deliver the oxygen and nutrients required to heal even the smallest scratch. What might take a few days to heal for someone without diabetes could take weeks for someone living with the condition, increasing the window of opportunity for infection.
The 60-Second Daily Diabetic Foot Check
- Check the Tops: Look for any new redness, swelling, or unexplained bruising.
- Check the Soles: Use a mirror if you have limited mobility to look for blisters or cuts on the bottom of your feet.
- Feel the Temperature: Run your hand over both feet. Do they feel unusually hot (a possible sign of infection) or very cold (a sign of poor circulation)?
- Inspect Between Toes: Look for white, soggy skin or breaks, which can lead to fungal infections.
- Check for Blisters: Even small “friction” bubbles need to be monitored closely.
- Inspect Your Shoes: Before putting them on, shake them out to ensure there are no grit, small stones, or sharp objects inside.

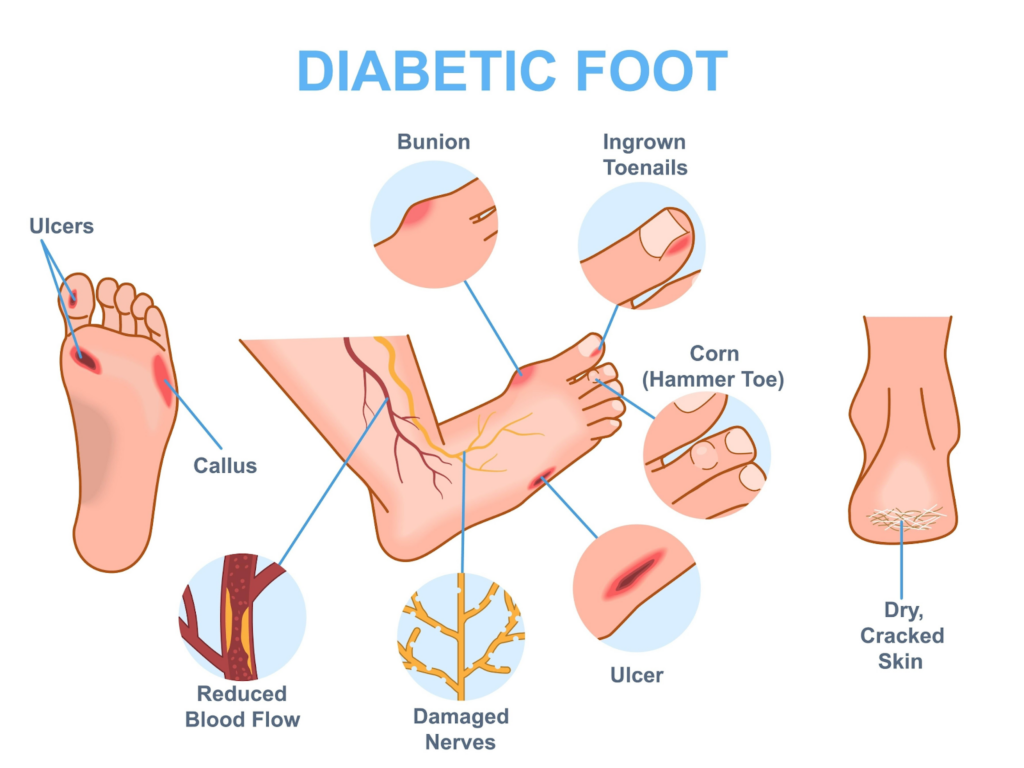
Common Problems to Watch For
- Callus and Hard Skin: This can act like a “stone in a shoe,” creating high-pressure points that eventually break down into ulcers underneath.
- Nail Issues: Thickened or ingrown nails can cut into the surrounding skin, leading to infection.
- Fungal Infections: Discoloured nails or itchy skin (Athlete’s Foot) should be treated promptly.
- Dry Skin and Fissures: “Cracked heels” serve as entry points for bacteria.
- Deformities: Changes in foot shape (like bunions or hammer toes) can create new pressure points.
Daily Habits: The Do’s and Don’ts
| Activity | ✅ The “Do’s” (Safe Habits) | ❌ The “Don’ts” (Avoid) |
|---|---|---|
| Cleaning | Wash daily with lukewarm water & mild soap. | Avoid very hot water or prolonged soaking. |
| Drying | Pat dry gently, especially between the toes. | Never leave skin damp between the toes. |
| Moisturising | Apply urea-based cream to the tops and soles. | Never put cream between the toes. |
| Protection | Always wear socks and supportive shoes/slippers. | Never walk barefoot (indoors or outdoors). |
| Nail Care | Cut nails straight across or use an emery board. | Never cut corners or use sharp “bathroom surgery” tools. |
| Heat | Use socks to keep feet warm at night. | Never use hot water bottles or heating pads on your feet. |
Red Flags: When to Seek Urgent Help
- A wound, blister, or cut that is not healing.
- Redness spreads away from a sore area.
- Pus, oozing, or an unpleasant smell from a wound.
- Part of the foot is turning black, blue, or very pale.
- Sudden, unexplained swelling or warmth in one foot.
Understanding Professional Support
| Feature | Foot Health Practitioner (FHP) | Podiatrist (Chiropodist) |
|---|---|---|
| Primary Focus | Routine maintenance & preventative care. | Complex medical issues & high-risk pathologies. |
| Common Tasks | Nail cutting, callus removal, and corn management. | Ulcer debridement, nail surgery, and biomechanics. |
| Diabetes Role | Monitoring & maintaining “low to medium risk” feet. | Annual screenings & managing “high risk” complications. |
| When to See Them | Every 6–12 weeks for steady foot comfort. | For annual medical reviews or active infections. |
Conclusion
Diabetic foot care is about empowerment through routine. By spending 1 minute a day checking your feet and adopting simple habits, such as moisturising and wearing sensible shoes, you can significantly reduce your risk of serious complications.
Whether you are in Lindfield, Cuckfield, or Burgess Hill, staying connected with your local footcare team ensures you remain active, mobile, and healthy.
Frequently Asked Questions
Why shouldn’t people with diabetes put cream between their toes?
Putting moisturizer between the toes creates a damp, dark environment that encourages fungal infections and “maceration” (soggy skin). This can cause the skin to split, creating an entry point for bacteria that may lead to a serious infection or ulcer.
How often should a diabetic person see a foot specialist?
According to NICE guidelines, people with diabetes should have a professional foot screen at least once a year. However, if you have calluses, thick nails, or reduced sensation, seeing a Foot Health Practitioner every 6–8 weeks is recommended to prevent minor issues from escalating.
What are the first signs of diabetic foot problems?
Early warning signs include tingling or numbness (pins and needles), skin that feels unusually hot or cold to the touch, and small cuts or blisters that do not show signs of healing within 24–48 hours.
Content Assurance & Governance
- Reviewed By: The Clinical Team at Borde Hill.
- Evidence Base: Data sourced from Diabetes UK (2025/2026 reports) and NHS Digital.
- Compliance: This article aligns with NICE (National Institute for Health and Care Excellence) guidelines [NG19].
- Last Updated: March 17, 2026.